IASR 42(5), 2021【THE TOPIC OF THIS MONTH】Enterohemorrhagic Escherichia coli (EHEC) infection as of March 2021 in Japan

The topic of This Month Vol.42 No.5(No. 495)
Enterohemorrhagic Escherichia coli (EHEC) infection as of March 2021 in Japan
(IASR Vol. 42 p87-88: May 2021)
Enterohemorrhagic Escherichia coli (EHEC) infection is caused by E. coli that produces Verotoxin/Shiga toxin (VT/Stx) and/or possesses VT-encoding genes. The main signs/symptoms of EHEC infections are abdominal pain, watery diarrhea, and bloody diarrhea. Vomiting and/or fever (≥38°C) are occasionally observed. VT-producing EHEC can cause hemolytic uremic syndrome (HUS), which involves thrombocytopenia, hemolytic anemia, and acute kidney injury; complications, such as encephalopathy, may also occur, with potentially fatal outcomes.In Japan, EHEC infections are classified as a category III notifiable infectious disease under the Infectious Diseases Control Law. When a physician diagnoses EHEC infection, they must immediately notify a local public health center (PHC) regarding the case (http://www.niid.go.jp/niid/images/iasr/37/435/de4351.pdf). The information collected by the PHC is then reported to the National Epidemiological Surveillance of Infectious Diseases (NESID) system. When an EHEC infection is classified as food poisoning by a physician or the director of the PHC, the local government investigates the incident and submits a report to the Ministry of Health, Labour and Welfare (MHLW) in compliance with the Food Sanitation Law. Prefectural and municipal public health institutes (PHIs) perform isolation/identification of EHEC, serotyping of the isolate, and typing of the VT (the VT or the VT gene), and report the laboratory results to Infectious Agents Surveillance System under the NESID system (see p.89 of this issue). The Department of Bacteriology I of the National Institute of Infectious Diseases (NIID) conducts confirmatory tests upon request, and conducts molecular epidemiologic analysis of EHEC using multiple-locus variable-number tandem-repeat analysis (MLVA) and pulsed-field gel electrophoresis (PFGE) (see p.96 and 97 of this issue). The results of the analysis are fed back to the PHIs and, when necessary, to local governments through the National Epidemiological Surveillance of Foodborne Disease (NESFD) system.
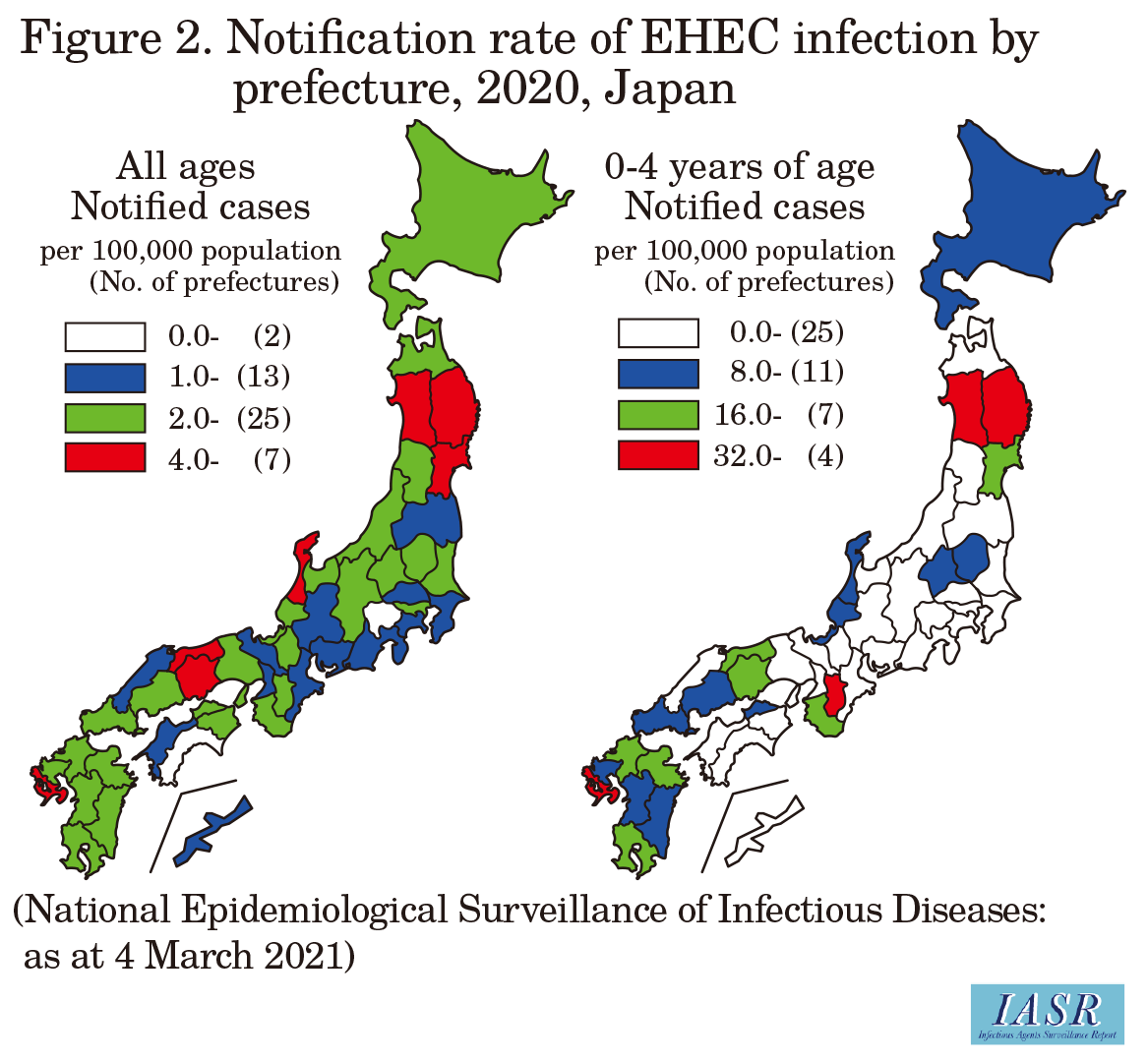
Cases notified under the NESID system
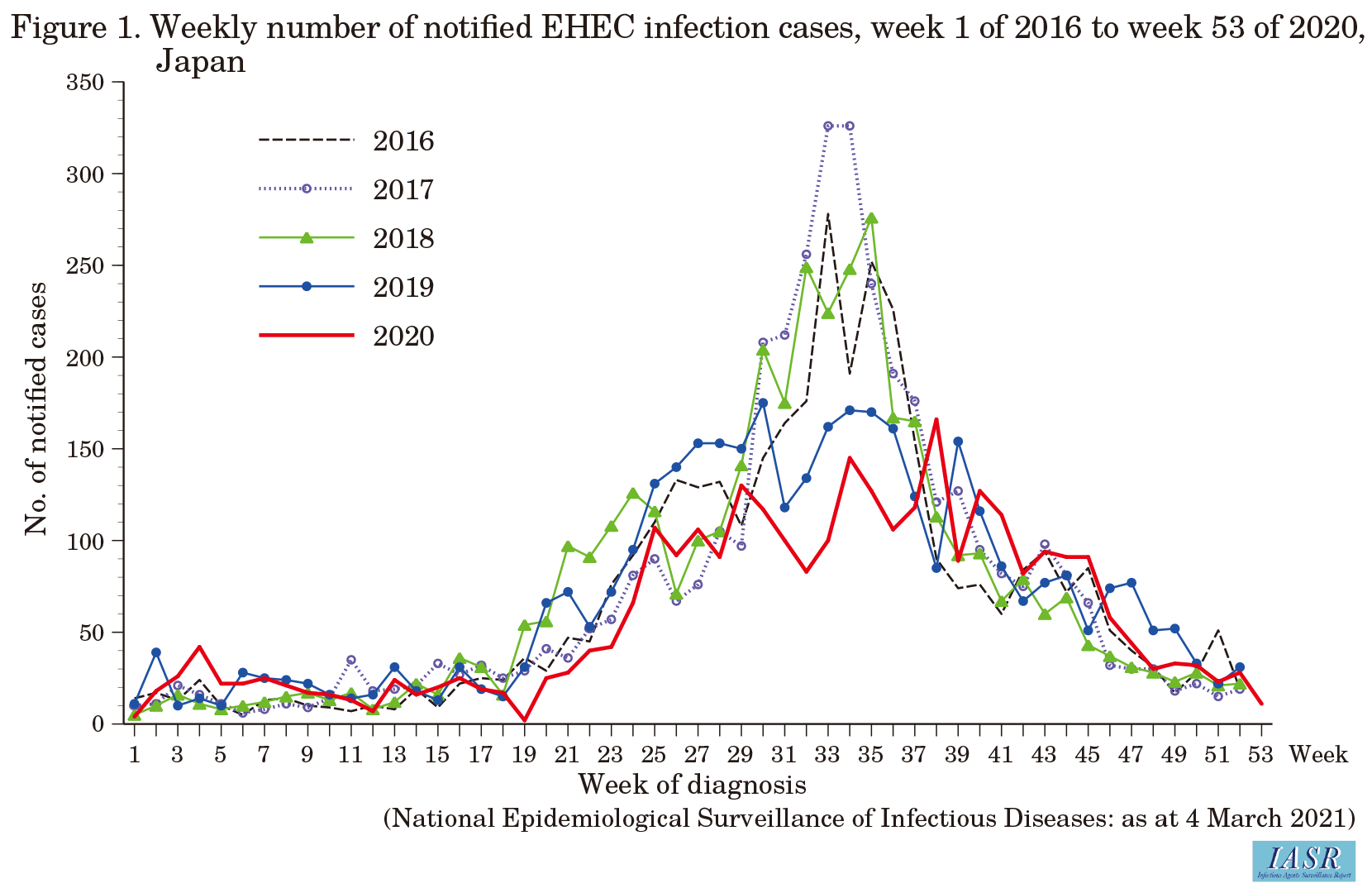
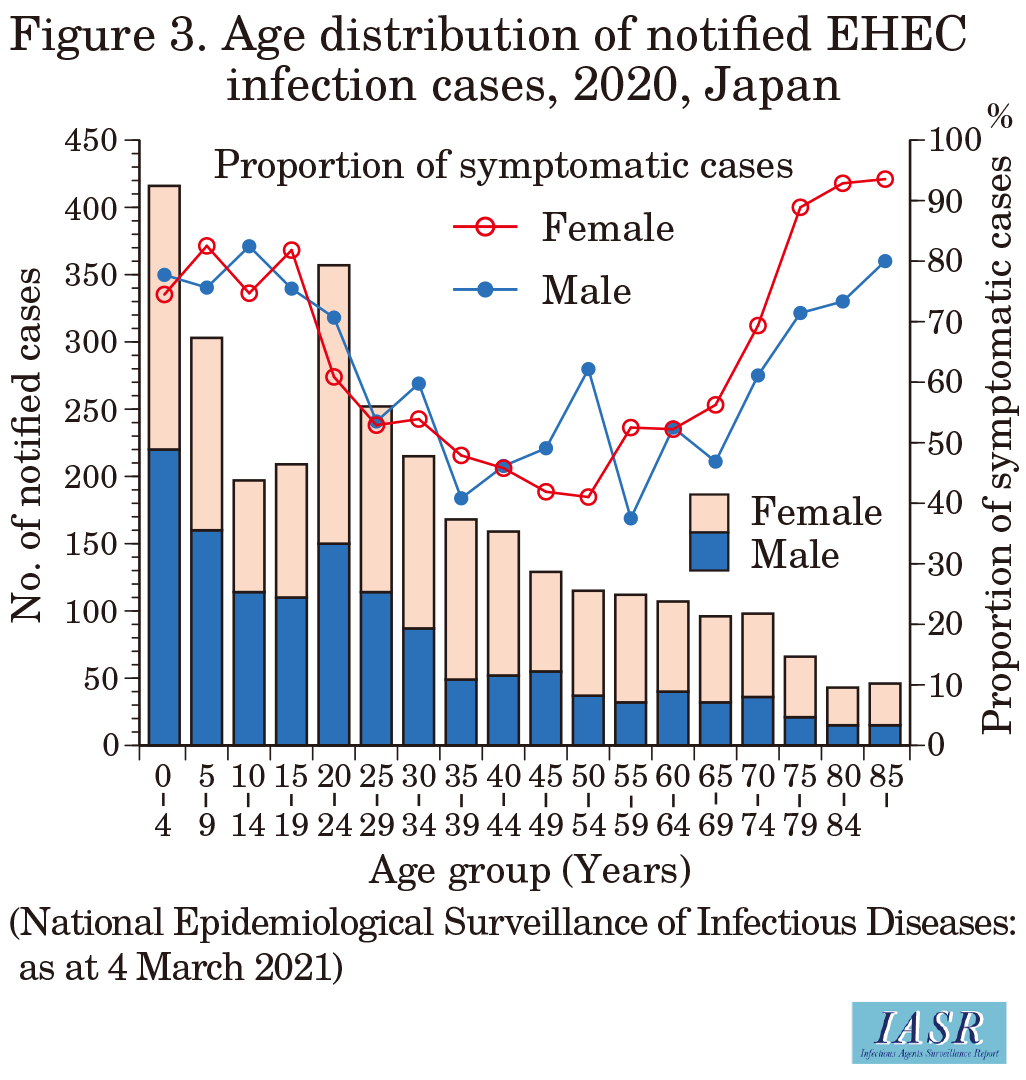
According to NESID, in 2020, a total of 3,088 cases of EHEC infection were reported, including 1,985 symptomatic patients and 1,103 asymptomatic carriers (asymptomatic cases are detected during active epidemiologic investigations or routine stool specimen screening of food handlers) (Table 1), which was 80.3% of the 3,847 average cases reported between 2011 and 2019. Consistent with previous years, the number of cases peaked in summer (Fig. 1), but there were more reported cases in 2020 than in 2016-2019 in calendar weeks 38-45. Reports from the top 10 prefectures with the most notifications, Tokyo, Fukuoka, Kanagawa, Hokkaido, Osaka, Aichi, Chiba, Nagasaki, Hyogo, and Miyagi, accounted for 51.5% of all notified cases (including asymptomatic cases). The annual number of notified cases per 100,000 population was highest in Akita Prefecture (10.1), followed by Nagasaki (8.9), Iwate (6.0), and Okayama (5.4) Prefectures (Fig. 2 on p.88). The notification rate per 100,000 population among 0-4-year-olds was highest in Nagasaki Prefecture (90.4), followed by Akita (88.9) and Iwate (50.0) Prefectures (Fig. 2 on p.88). The proportion of symptomatic cases among notified cases was high among the <20-year-old and ≥70-year-old age groups in both males and females (Fig. 3 on p.88).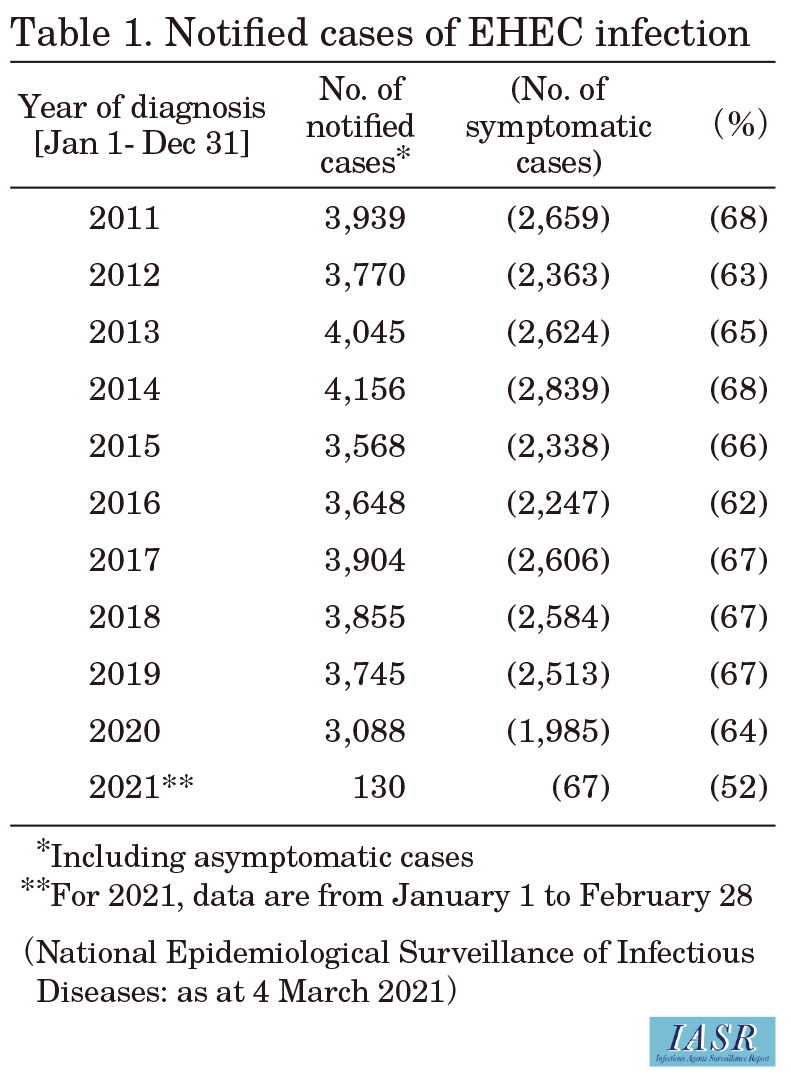
Among the 64 cases complicated by HUS (3.2% of symptomatic cases), EHEC was isolated from 34. The O-serogroup was O157 in 25 cases and the toxin type was VT2 (VT2 alone or VT1 & VT2) in 21 cases. Among the symptomatic cases, HUS was most frequent in 5-9-year-olds (7.1%), followed by 0-4-year-olds (5.7%) (see p.98 of this issue). At the time of notification, there was one case of death due to EHEC infection. In 30-40% of HUS cases, EHEC is not isolated, and detection of toxin in the stool or the detection of agglutinating antibodies against the major O group of EHEC in the blood by serodiagnosis confirms the diagnosis of HUS due to EHEC infection (see p.99 of this issue).
EHEC detection reported by PHIs
In 2020, PHIs detected 1,422 cases of EHEC (see p.89 of this issue). This figure is lower than the number of notified cases of EHEC infection (Table 1 on p.87) because this number represents the number of detected strains submitted by medical facilities and commercial laboratories upon requests by the PHCs. The most frequently detected O-serogroup was O157 (47.2%), followed by O26 (21.4%) and O103 (9.8%) (see p.89 of this issue). In terms of toxin types, in 2020, VT1 & VT2-positive was the most common for O157 as in previous years, accounting for 60.7% of O157, and VT2-positive accounted for 38%. For O26 and O103, VT1-positive was the most common as in previous years, accounting for 96.4% and 97.9%, respectively. The main clinical signs/symptoms among the 671 cases in which O157 was isolated were diarrhea (59.6%), abdominal pain (58.6%), bloody diarrhea (43.8%), and fever (18%).Outbreaks
As in past years, EHEC outbreaks at nursery schools and other locations occurred in 2020, and they were presumed to be due to person-to-person transmission (Table 2, see p.92 and 93 of this issue). Five EHEC-related food poisoning outbreaks, with a total of 30 patients, including EHEC isolation-negative cases, were reported based on the Food Sanitation Law (17 outbreaks involving 156 cases in 2017; 32 outbreaks involving 456 cases in 2018; 20 outbreaks involving 165 cases in 2019) (see p.90 and 91 of this issue). The analysis by the Department of Bacteriology I of the NIID revealed that strains exhibiting the same MLVA type among sporadic cases of unknown epidemiologic association were isolated from a wide geographic area (see p.96 and 97 of this issue).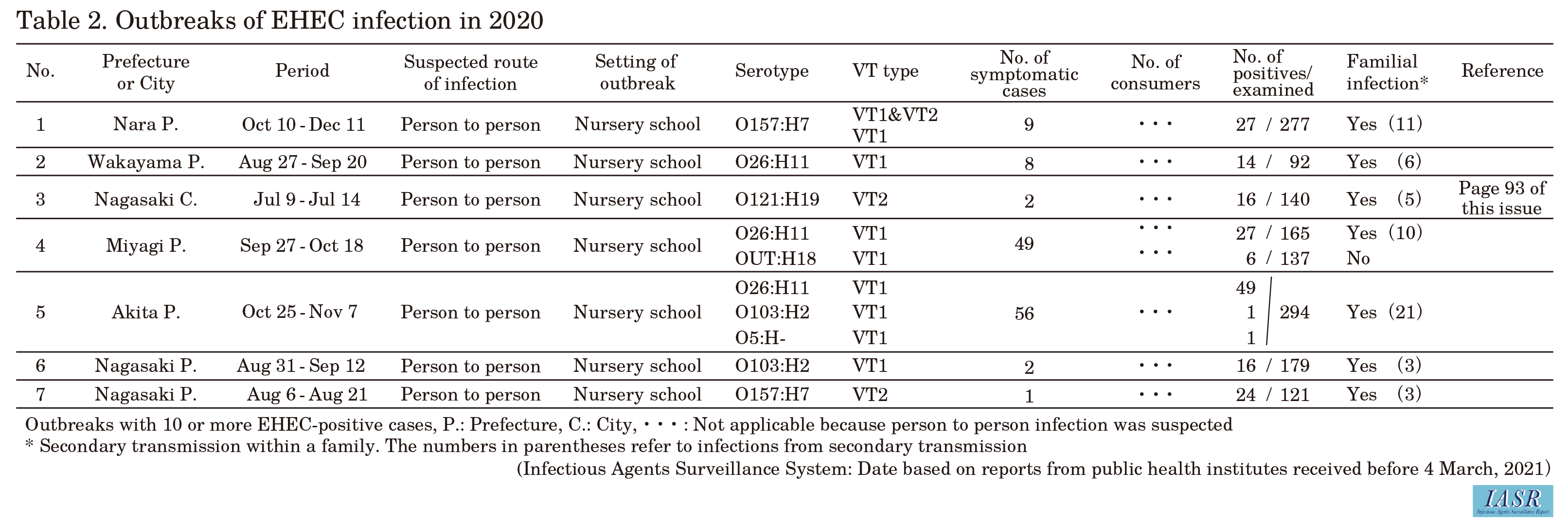
Prevention and measures to be implemented
In response to food poisoning events caused by raw beef, the MHLW revised the standards for beef sold for raw consumption (MHLW notice No. 321, October 2011). Furthermore, upon the detection of EHEC O157 from the inner section of cattle liver, the MHLW banned the sale of beef liver for raw consumption (notice No. 404 in July 2012). In 2012, in response to O157-based food poisoning outbreaks attributed to contaminated pickles, the MHLW revised the hygiene code for processing pickles (food safety inspection notice 1012, No. 1, October 2012).As EHEC can cause infection at bacterial counts as low as ~100, it can easily spread via person-to-person transmission or person-to-food ingredients/products. EHEC-associated food poisoning events attributed to restaurants occurred in 2020 as in past years (see p.90 of this issue). To prevent EHEC infections, it is essential to observe the principles of proper food hygiene and continue risk communication activities aimed at reducing the consumption of raw or undercooked meat.
Furthermore, EHEC outbreaks continue to occur in large numbers in nursery schools. To prevent such outbreaks, appropriate hygienic practices, such as routine hand washing and hygiene management at swimming pools, should be implemented (“Infection Control Guidelines for Nurseries” revised in 2018). When a case of EHEC infection is detected within a household or care facility, the PHC should ensure that appropriate measures are strictly implemented to prevent further transmission.

