Erythema infectiosum, Epidemiological week 1-25, 2025( as at June 25th 2025)
![]()
![]()
◆Erythema infectiosum, Epidemiological week 1-25, 2025( as at June 25th 2025)
Erythema infectiosum is an epidemic-prone exanthematous disease caused by human parvovirus B19 (HPV-B19), primarily affecting children. It is transmitted mainly through droplet or contact transmission, and spreads via outbreaks in settings such as childcare facilities and schools. The virus is also spread via secondary transmission within households. Characteristic symptoms include well-defined erythema on both cheeks appearing after an incubation period of 10–20 days, followed by bilateral, reticular or lace-like rashes on the limbs (see photos 1 and 2: https://id-info.jihs.go.jp/diseases/ta/5th-disease/010/5th-disease.html). In typical cases, the cheeks become as red as apples, which is why the disease is referred to as “apple disease” in Japan. Before the appearance of erythema, patients may exhibit cold-like symptoms such as fever and sore throat, and they are considered highly infectious during this period. However, individuals are generally no longer considered infectious by the time the erythema and rash appear. About a quarter of infections are asymptomatic, and even symptomatic cases generally have a favorable prognosis. However, infection in a pregnant woman with HPV-B19 during early to mid-pregnancy can result in transplacental transmission of HPV-B19 to the fetus, which may cause severe complications such as miscarriage, stillbirth, or fetal hydrops. In addition, in patients with hemolytic anemia such as sickle cell disease, infection can cause aplastic crises. In immunocompromised individuals, the infection can cause severe, chronic anemia and requires careful monitoring. There is no specific treatment or vaccine; only supportive care, such as observation and antipyretic/analgesic therapy, is available.
Under Japan’s Infectious Diseases Control Law in effect since 1999, erythema infectiosum is classified as a Category V pediatric sentinel surveillance disease in the National Epidemiological Surveillance of Infectious Diseases (NESID). Pediatric sentinel medical facilities report the weekly number of cases by sex and age group when physicians clinically suspect the disease and observe erythema on both cheeks and lace-like erythema on the limbs. The number of reported cases divided by the number of reporting sentinel sites is referred to as “reported cases per sentinel site,” and this indicator is used to monitor disease activity trends.
Surveillance for erythema infectiosum began in 1982. Major epidemic years before the enactment of the Infectious Diseases Control Law were 1987, 1992, and 1997. After the law came into effect in 1999, large epidemics occurred in 2001, 2007, 2011, and 2015, showing a cyclical pattern with major epidemics being observed approximately every 4 to 6 years. In epidemic years, peaks were typically observed around June to July (between weeks 23 and 27), but such seasonality has become less clear in recent years. The last epidemic year before the COVID-19 pandemic was 2019. From the start of the COVID-19 pandemic through 2023, the weekly number of reported cases per sentinel site remained low, below 0.02 throughout the year without major epidemics.
In 2024, the levels remained low through week 19, but began to increase afterwards, reaching 0.56 cases per sentinel site (1,742 reported cases) in week 46. The upward trend continued, and in week 51, the number rose to 0.98 (3,076 reported cases). In 2025, the number remained at a similar level early in the year but decreased to around 0.6 from week 6, then rose again to 0.81 (2,516 reported cases) in week 11. In week 20, cases per sentinel site reached 2.05 (4,834 reported cases), marking the highest level since the current surveillance system was introduced in 1999. In week 25 (as at June 25, 2025), the number further increased to 2.53 cases per sentinel site (5,943 reported cases). It should be noted that in week 15 of 2025, the Implementation manual for the National Epidemiological Surveillance of Infectious Diseases Program was revised in conjunction with the launch of the Acute Respiratory Infection Surveillance. This revision changed the criteria for selecting sentinel sites, reducing the number of pediatric sentinel sites nationwide from approximately 3,000 to 2,000.
By age group, prior to the COVID-19 pandemic, the highest proportions of cases were observed in children aged 3–5 years or 6–9 years. During the COVID-19 pandemic (2020–2023), the number of reported cases decreased across all age groups, with a more pronounced decline among children aged 3 years and older (Table 1). Since 2024, the age distribution trends have returned to the pre-pandemic pattern.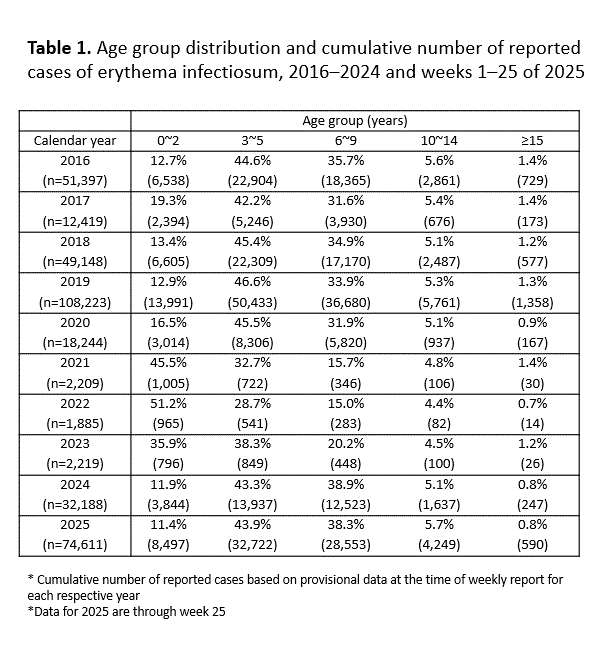
As at week 25 of 2025, prefectures with the highest number of reported cases per sentinel site were Yamagata (7.62), Gunma (7.32), Tochigi (7.26), Nagano (6.04), and Toyama (5.38). The cumulative numbers of reported cases per sentinel site for weeks 1–25 were highest in Tochigi (70.87), Yamagata (70.32), Fukushima (61.62), Toyama (51.64), and Hokkaido (51.08). Conversely, prefectures with the lowest respective values were Tokushima (3.59), Okayama (4.57), Kagawa (5.67), Kagoshima (7.80), and Yamaguchi (7.88). Overall, reported cases per sentinel site were particularly high in regions north of the Kanto area. Regarding the regional trends in erythema infectiosum activity over the years, the number of reported cases per sentinel site tended to rise first in the Kanto region, with a spread to other regions following during epidemic years. In the increase observed from autumn 2024 onward, the Kanto region again showed an earlier rise, followed by a nationwide increase. As at week 25 of 2025, the regions with the next highest number of reported cases following Kanto were Hokkaido and the Tohoku region (Table 2).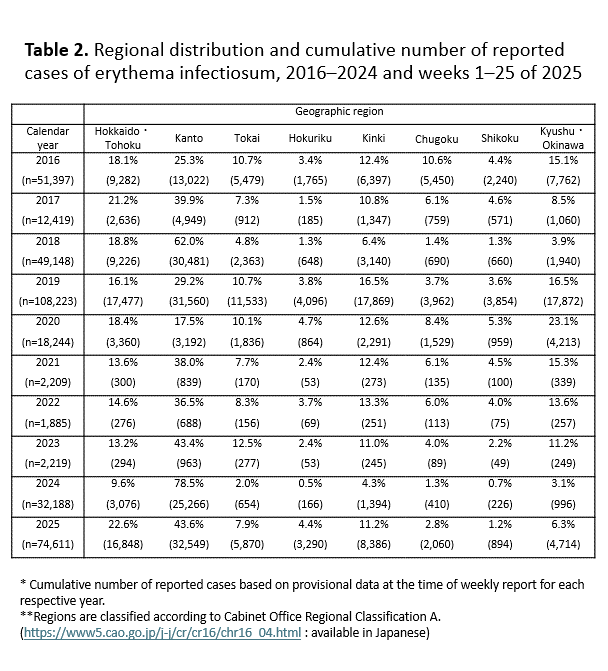
Since a certain proportion of erythema infectiosum infections are asymptomatic, it is likely that there are infected individuals in addition to the reported cases. During the erythema phase, the infectivity is minimal. However, individuals are not usually diagnosed during the preceding infectious period as they do not present characteristic symptoms, which make prevention efforts challenging. It is important to provide information on the erythema infectiosum activity situation to pregnant women and individuals with underlying conditions such as hemolytic anemia or immunodeficiency, as infection in these groups may lead to severe complications. Moreover, such individuals should take precautions when caring for a child who is unwell or when in contact with a group of children, including thorough hand hygiene, avoiding the sharing of utensils, and wearing masks. Since erythema infectiosum historically tended to show increased activity levels from early to mid- summer, continued monitoring of disease activity trends is necessary, even in areas where large outbreaks have not yet been observed as at week 25.
- Erythema infectiosum (Fifth disease) (NIID, JIHS)
https://id-info.jihs.go.jp/niid/ja/kansennohanashi/443-5th-disease.html - Erythema infectiosum (Human parvovirus B19 infection), IASR Vol. 37, No.1 Jan 2016
https://id-info.jihs.go.jp/niid/ja/typhi-m/iasr-reference/6285-iasr-431.html - Notable Infectious Diseases: Erythema infectiosum, IDWR Week 26, 2015
https://id-info.jihs.go.jp/surveillance/idwr/idwr/2015/idwr2015-26.pdf - Notable Infectious Diseases: Erythema infectiosum, IDWR Week 14, 2019
https://id-info.jihs.go.jp/idsc/niid/images/idsc/idwr/IDWR2019/idwr2019-14.pdf - David L. Heymann (edit). Erythema Infectiosum. Human Parvovirus Infection (Fifth disease). Control of Communicable Diseases Manual 19th edition. 2008
- Erik D. Heegaard and Kevin Brown. 2002. Human Parvovirus B19. Clin. Microbiol. Rev. 15(3): 485-505.
Department of Infectious Disease Surveillance
National Institute of Infectious Diseases, Japan Institute for Health Security

